| A DIMENSIONAL INTERPRETATION OF PSYCHOTIC DISORDERS: FROM TYPICALITY TO ATYPICALITY |
Souza, G. F. J.*
*Psychiatric Physician
Supervisor for interns at "Hospital das Clínicas"
UFMG (Federal University of Minas Gerais)
SUMMARY
In this paper, by presenting two clinical cases, the author frames the concepts of psychotic typicality and atypicality and then compares atypical psychotic cases with the more typical ones, particularly those of schizophrenia. From this comparison, he develops a theoretical model which culminates in a diagrammatic representation of several nosologic unities belonging to the scope of endogenous psychoses, placing them within a specific spectrum according to their degree of typicality, greater or smaller. The author believes these theoretical considerations can enhance the psychiatric semiologic tools which would enable physicians to face the diagnosis and treatment of atypical psychosis more confidently and accurately.
INTRODUCTION
The management of general psychotic manifestations in daily practice provides us with several examples of psychiatric pictures which are phenomenologically atypical and, to a certain extent, nosologically intriguing. When facing those cases, any psychiatrist will, at first, naturally turn his/her thoughts towards those classic psychotic cases whose psychopathological contents are already well established and outlined, that is, the typical ones, looking for any phenomenological similarity between them as they are inevitable, compulsory clinical references. However, in many cases, patients report such amazing anomalous experiences and show such unexpected and unpredictable clinical history that the physician is unable to recognise, at least initially, the actual nosological nature of those cases and limits him/herself to treat only its symptomatological nature, harming the effective control of the disease considerably and delaying the patient’s resocialisation. Therefore, I believe it is necessary to establish new theoretical-practical references to enable us to account for and explain some psychopathological configurations which, despite being atypical, are phenomenologically well described and consolidated. With this aim in mind, we start this paper presenting two clinical cases of atypical psychosis and then will engage in a theoretical discussion about them, aiming towards a dimensional interpretation of general psychotic disorders.
CASE REPORTS
Clinical Case I (20):
W., 17 years old, female, single, student (primary school concluded).
She lived in Belo Horizonte with her oldest sister. Her parents had separated three years before. The family contacted me in July of 1989 asking for an urgent appointment.
According to her sister, in the previous week, the patient had started showing changes in her behaviour. One morning, she had turned up in an evening dress, claiming that she was dressed like that to receive her father that, according to her, would arrive at any moment (which was not true). In addition, she would have childish behaviour, baseless fears, insomnia, restlessness and agitation, being calmed down after great effort.
When examined, she showed a kind of mischievous puerilism, coming into my office skipping and hopping, greeting me with a curious childish inflection in her voice. She could not remain sitting for more than some seconds, showing inattention and restlessness. Her facial expression conveyed distress, anxiety, discomfort, fear and her feet and hands fidgeted uncontrollably like a child. She said she had been missing her "papa" and was scared as she had been having "visions of ugly faces like monsters" (sic). There were no evidences of delusional or hallucinatory activity in the examination, her attention was hyper-vigilant and hypo-tenacious in a sort of uncalm, absent-mindedness and her thoughts, memory, consciousness and consciousness of the ‘ego’ seemed intact.
Personal Background (P.B.): irregular use of marijuana, no history of seizure or any other significant disease, failure in several exams at school, inconstant and disturbed love life.
Family Background (F.B.): mother with recurrent depressive disorder (chronic monopolar disorder); one of her brothers and an maternal aunt with potential psychotic picture.
Therapeutic Procedures:
She was prescribed pericyazine at 40 to 60 mg/day. After 48 hours, as there was no improvement, she was taken to hospital immediately. During that time, 15 days, she was given 25mg of fluphenazine depot associated with 15 mg of haloperidol/day and 200 mg of chlorpromazine/day. The acute picture was entirely reverted.
In May of 1990, she came back to my office along with her relatives displaying symptoms suggesting prodrome of another crisis similar to the previous one. She had given up the medicines prescribed previously and five days before had started showing restlessness and insomnia again as well as imprecise and vague fears. She was prescribed pipothiazine depot (1 ampule of 25 mg, intramuscular) associated with 40 mg/day de pericyazine and after one week, her sister informed me she was much better.
I had not heard from that patient until 03/Dec/91 when she came back to my office showing loss of movement as well as being rather scared, frightened and sleepless. I prescribed pipothiazine depot (50 mg, intramuscular) and asked her to return the following week. By that time, she was fine, syntonic, and moving normally, but crying very easily and showing affective lability. I added amitriptyline (75 mg/day) and after some days, she reported a considerable improvement. After that episode, the patient did not return to treatment and I didn't hear about her until recently, nearly nine years later, when I learned she had married and had two children. She had had other crises, apparently depressive, followed by restlessness and worsened by regular use of marijuana.
General Impression: There were some personality traits, identified by studying her past life, compatible with "Borderline Personality Disorder" and "Histrionic Personality Disorder", as in DSM-IV (3).
Diagnosis Hypothesis (D.H.): Atypical psychotic picture in a patient with personality disorder.
Clinical Case II (19):
V., female, 32 years old, single, teacher graduated in History.
In November of 1989, she showed a depressive picture with regular episodes of depersonalisation and derealisation, in addition to explosiveness and aggressiveness crises towards members of her family. They reported that the patient would lock herself in her bedroom most of the time and, when she did come out, would insult and threaten everyone, particularly her brother-in-law who had never done any harm to her. Alternately to her choleric outbursts, she would cry continuously and convulsively and, at times, showed a disturbed appearance with a brightly fixed eye expression, refusing to talk to anyone. On those occasions, while feeling apart from the outside world, she was a prey for great distress and anxiety and some unpleasant events of her biographic past, most of them devoid of decisive importance in her life, would occupy her psyche in an obsessive, repetitive, persistent way, leading to great personal suffering. Despite great effort, she could not help thinking about them and would gradually live an unusual hatred towards some members of her family as well as highly aggressive and harmful impulses and fantasies which, occasionally, led to noisy choleric outbursts and impetuous arousal that took everyone by surprise.
In V.'s first examinations and subsequent interviews, I could not notice any delusional and/or hallucinatory activity, her consciousness was clear, her language was characterised by rich verbal fluency, her thought and other psychic functions seemed rather normal. My impression was that she was very shy and reserved, but I could notice a singular affective coldness in her reportings, including those which must induce important emotional mobilisation. In a way, it was reinforced by a slight affectation which coloured her speaking and her gestural spontaneity was mildly deadened by a vague mechanical connotation. This display of lack of spontaneity was reinforced by her eye expression and mime, both showing little expressivity. However, I could not find significant incoherence or disagreement in her affective syntony, apart from a mild weirdness sensation hovering in her verbal contact.
Personal Background (P. B.): Several psychiatric treatments since her adolescence, including ECT under narcosis and curarization at the age of 17 as an out-patient. Natural childbirth at full term, simple Common Childhood Illnesses, no history of seizure or any other significant disease; contemplative and introvert temper, excessive shyness in childhood and adolescence; scarce love life. Bound to have been dysthymic since childhood.
Family Background (F.B.): Several cases of psychiatric disorders in her family, probably, compatible with major depression, dysthymia and personality disorders; father diagnosed as "schizophrenic", although, apparently, he does not show any visible loss in his social and family life.
Therapeutic Procedures:
At the beginning of the treatment, she was prescribed imipramine (50 mg/day), which she did not tolerate as her anxiety and restlessness worsened. As a second choice, she was given maprotiline at the dosage of 75 mg/day, with very few favourable results. At the peak of her crisis, I prescribed pipothiazine depot (1 intramuscular ampule of 25 mg fortnightly) and the clinical results were amazingly positive from the third day after she had started taking the medicine. Thirty days later, maprotiline was replaced by clomipramine (50 mg/day) and after that her clinical picture improved considerably. She was calm, co-operative and her crises and anomalous experiences vanished, including the episodes of depersonalisation and strangeness of "the noticed". Thus, V. is now balanced and has been taking only paroxetine at a dosage of 40 mg/day for about five years.
General Impression: There were some personality traits, identified by studying her past life, compatible with "Borderline Personality Disorder" and "Schizoid Personality Disorder", as well as dysthymia, according to DSM-IV (3).
Diagnosis Hypothesis (D.H.): Atypical psychotic picture in a patient with personality disorder.
CLINICAL DISCUSSION AND THEORETICAL CONSIDERATIONS
W.'s first acute crisis was clinically manageable, however, it could not be considered as perfectly fit in a typical manic phase. On the other hand, a clear depressive tone mingled with her hyperkinetic puerile behaviour was visible and a closer examination of her anomalous experience revealed, besides a clear tachypsyche, feelings of a melancholic nature, such as apprehension, dismay and fear. Her second acute crisis, exactly a year later, was clearly depressive in character, but, similar to the first one, did not fit into the diagnostic criteria to be regarded as a typical depressive phase. It can be said that her acute symptoms consisted of modes of anomalous experiences composed by depressive and manic elements occurring simultaneously and a frustrated and disappointing character (18) , hence implying its atypical and uncharacteristic aspect. That was confirmed by her favourable therapeutic response to an incisive neuroleptic and, subsequently, to its association with an antidepressant. W.'s temporal clinical development happened favourably and benignly. Nevertheless, some psychopathological aspects of her clinical picture need to be better explained. I believe that can be done more clearly after discussing V.'s case and the theoretical considerations which follow.
V. showed a tendency to introversion, seeking refuge inside herself, in her imagination, daydream and fantasies as well as had been revealing a clear liability to solitary behaviour since childhood. According to her, she had been an excessively shy, withdrawn and frightened child. She could remember that, in her childhood, she hardly took part in any games and amusements children of the same age did. In addition, she was too scared of everything and subjected to frequent crises of night terror and crises of nervousness. She said that she had been an extremely sensitive and impressionable girl and most of the time would prefer to play on her own, steeped in an universe richly inhabited by weird beings and imaginary fellows. In early puberty, she began suffering intense depressive crises and that is when she started undergoing psychiatric treatments, which she would need for the rest of her life. Besides this clear personality vulnerability, she would, in contrast, have a rich intellectual life and highly refined cultural interests. Since early age, she was keenly interested in the Arts, showing a special gift for drawing, as well as a singular curiosity for Humanities and Philosophy which matched very well with her contemplative and aesthetic temperament. As expected, she had a dense inner life, naturally guided towards reflection, but at the same time, disturbed by several conflicts, doubts, lack of confidence and hesitations. Her social life had always been troublesome and difficult, from her adaptation in work groups at school to love and personal relationships. She did not trust anyone, and was withdrawn and extremely susceptible to the slightest signs of disapproval or rejection. On the other hand, she was tender and altruistic, valued and kept her appointments and responsibilities seriously and correctly and was rather worried about her family's problems. Her professional life was at risk due to frequent disagreements with her colleagues in the various jobs she had had. Moreover, since a serious nervous breakdown she suffered while living abroad for a post-graduation course, she had limited herself to making plans and projects which have never been carried out. However, when her crises aroused, she would become extremely choleric, explosive and irritable, withdrawing from everybody and displaying an apparently motiveless feeling of hatred. Lately, she had been experiencing long periods of feelings and states of mind marked by apathy and impassivity and, at times, a cold and apathetic indifference. On other occasions, when an acute crisis approached, she experienced a tendency to irritability, annoyance and nervousness along with strong and mobilising emotions associated with vivid images of her childhood and adolescence.
It seems likely, after describing those two clinical cases, that both correspond to atypical psychotic cases in patients with personality disorder. Those atypical pictures, which in our opinion would be defined better if they were called psychoid states (18), seem to consist of diverse psychopathological expressions corresponding to frustrated and abortive symptoms of typical and well-defined psychotic pictures. The terms typical and atypical would in turn refer to the concept we intend to frame, that is, maximum psychotic typicality and atypicality.
By maximum psychotic typicality, we mean that level of psychopathological expression in which, in a lateral section of the phenomenological report, all typical schizophrenic symptoms are included, whether predominantly positive or negative (26). In a longitudinal section, its usual and known, unfavourable clinical development which inevitably leads to a psychic deterioration condition or processual defect (8,7), after successive appearance of psychotic episodes. In short, the highest degree of psychotic typicality includes, besides the morphologically typical and unmistakable psychopathological aspects of schizophrenic episodes or outbreaks in its acute and productive phase, the progressive and fatal damage of the patient's affective-symbolic dimension (22) during the clinical development of the disease. Thus, in the maximum psychotic typicality pole, there are those anomalous experiences so well described and classified by classic authors, such as "echo", "stealing" and "broadcasting" of thoughts, phenomena of influence and audible hallucinations by means of dialoguing "voices", among others (6,17,5). However, those specific psychopathological symptoms should belong to the maximum pole of psychotic typicality only if they coexist with an unfavourable clinical history typical of schizophrenia. It can be noticed that I have mentioned the term "affective symbolic dimension" and it refers to a clinical-empirical concept we have previously established and which can be very useful in practice, that is, the notion of affective symbolic dis-differentiation (22). In our opinion, that alteration seems to be an axial characteristic of an schizophrenic disorder and leads to the emergence of some modes of phylogenetically archaic symbolisation (22) that saturate the processes of superior psychic integration of an indelible character of reification. By reification, we mean those archaic modes of animistic-magic nature, in other words, of concrete symbolism which colour and shape the delusional judgements and hallucinatory experiences so typical in schizophrenics. It is interesting to point out that as the disease develops, we can notice a kind of fading of individual character traits, progressive loss of those nuances and peculiarities of temperament and character, so particularly personal in all of us and which reflect the human singularity mark. The kraepelinan term dementia praecox suggests this phenomenon of emptiness of personality, loss of personal peculiarities associated with a cognitive deficit always present. The patient is thrown in a kind of archaic and empty universality, as he/she had been definitely deprived of the universe of symbolic diversity, of that plasticity involving the mildest, finest and subtlest personal differences. It crosses my mind, by means of comparison, the metaphoric image of a robust, evergreen tree with a green, lush top decorated with several colourful fruits and flowers which was slowly being destroyed vertically or descendingly. At first, it would lose its fruits and flowers, and then its leaves would become dull and lifeless, until it is reduced to a dry, rough trunk. The schizophrenic process also seems to attack the psychic life vertically and descendingly. Those more refined and singular personal attributes gradually vanish up to the point of resulting in what the German school of psychiatry called "brutalization" (verblödung) (8), meaning the deficient affective-cognitive aspect of patients with dementia praecox. Due to the irreversible damage of the superior modes of affective and symbolic integration resulting from the dis-differentiation process of those sectors, more archaic expressions of symbolisation are likely to emerge and occupy the entire psychic life in an archaic and definitive manner.
So we have considered the clinical prototype of maximum psychotic typicality, that is, schizophrenia. What about those atypical psychotic pictures we called psychoid states, illustrated by two clinical cases described above?
I believe it is reasonable to suggest, going back to the beginning of the theoretical discussion, that those atypical clinical pictures represent an incomplete and unsuccessful development of nosology corresponding to a typical mood disorder, whether depression or mania or, perhaps, even to a potentially schizomorph disorder. Thus, the clinical-psychopathological morphology of those pictures would correspond to abortive anomalous experiences steaming from typical schneiderian (17,6) or affective symptoms, or even from both coexisting simultaneously. Hence, considering this prevailing psychopathological expression corresponds to frustrated and abortive symptoms of well-defined psychotic pictures, it is not surprising its clinical development is also frustrated and atypical resulting in a favourable and benign clinical course. We can also see that most atypical psychotic cases develop on a pre-morbid and altered personality, and the difference between those patient's regular and lasting anomalous experience reactions and those formal features of psychoid states the patients display can eventually be phenomenologically detected (18). First of all, the anomalous experience reactions of patients with personality disorder, such as "affective instability", "intense and unsuitable anger", "marked change of basic mood and depression, irritability ... intense and unsuitable anger... chronic feelings of emptiness and annoyance..." gathered in DSM-III-R (4) as diagnosis criteria are subjective experiences marked by mild or intense personal suffering and manifest usually and regularly. Whereas in psychoid states, we notice a slight rupture of the individual's existential chain along with atypical acute symptoms, either prevailingly schizomorph or affective. In addition, in general, the phenomenological report of this existential rupture arouses in the observer a feeling of strangeness when facing something which sounds incomprehensibly incoherent at various levels, depending on how serious the case is.
In another paper (18), we have already framed the concepts of characterological "prism" or "filter" and primary and secondary "morbus" as fundamental constituent elements of the source of what we named psychoid states (18). At that time, we established a probable, and perhaps credible, theoretical model which can explain how the atypical psychopathological symptoms are formed, as they move away from the usually found classical phenomenological references. To sum up what has been established, we postulated that when a bipolar affective disorder, for instance, which corresponds to what we called primary "morbus", occurs in the characterological "filter" or "prism", it can trigger a sequence of secondary physio-pathological changes, the secondary "morbus", and as a result, produce a final morphology of the identified clinical-phenomenological facade (18). Therefore, in V.'s case, it is likely that a bipolar affective disorder, the primary "morbus", triggered and enlarged schizoid and schizotypal traits pre-existent in her characterological structure, that is, in her personality, and hence produced symptoms and anomalous experiences marked by a remarkably schizomorph content. So, her intense, sudden and apparently reasonless rage was provoked by painful memories of her past, which now come up in a clearly reified and persistent way under the domain of a depressive experience. As far as we know, the melancholic patient's thoughts generally gravitate monotonously around themes such as death, failure and blame, but in V.'s case, this distressing perseveration was steeped in remarkable disagreement and inappropriateness, making her behaviour weirdly unpredictable and incomprehensible (8). That explains the impression that her personal suffering did not fit harmonically in the syntonic chain of her existence, making the observer feel as if he/she was facing something preposterous and incoherent.
The same explanations are valid for the patient W., highlighting the outstanding clinical-phenomenological aspect of the patient's ontogenetic regression, up to the point of manifesting attitudes and feelings literally identical to the ones she had had at a certain period of her infant development.
When asked about what she had experienced in her first crisis, in which she displayed a rather childish and puerile behaviour, W. answered she could not remember her attitudes well and what had happened on that occasion, apart from the fact that images and scenes of her childhood, particularly those ones in which her father was present, started invading her consciousness massively and uninterruptedly. According to her, those memories referred to unpleasant facts of her past which brought about deep feelings of something missing, desertion and rejection, invaded her so vividly and continually that, in our opinion, they seemed a kind of ekmnesia (7,14). On the other hand, during her crises, W. was a prey for feelings of fear and terror and believed people could harm, hit and hurt her, and did not feel well at all and was frequently struck by a sudden conviction she would die and there was no way out. Thus, it seems that the phenomenological structure of those anomalous experiences were more similar to acute cognition or ideas of failure steeped in a feeling of imminence of concretization of a tragic event (21), typical of melancholic pictures, than to those atypical and diffuse delusional events and perceptions (17), despite the diffuse auto-referential of her clinical picture. Therefore, it is reasonable to assume that those psychopathological events have induced the aspects of the patient's unusual clinical display, making us think that she actually started experiencing her infant fears and fantasies in a reifiedly concrete symbolic dimension.
In order to supplement the discussion about W.'s case, it seems right to think that the final clinical morphology of her acute crises had resulted, as we have already claimed, from a basic mood disorder ¾ more precisely, the settlement of a mixed picture of depressive and hyperthymic symptoms twined in her experiences ¾ mediated by her characterological structure. In other words, the mixed affective disorder, the actual primary "morbus", when occurring in the characterological "filter" or "prism" containing prominent histrionic traits triggers a sequence of secondary physio-pathological changes, the secondary "morbus", and hence produces the final clinical morphology, that is, affective symptoms mixed with unsuitable and bizarre histrionic attitudes and experiences similar to a real "hysteric psychosis". Therefore, the histrionic component of personality would turn itself into something far beyond the characteristics exaggerated and amplified by the primary disorder. It would turn itself into a psychoid way of being (18), that is, in a clinical picture similar, in many ways, to endogenous psychoses, but displaying phenomenologically abortive and frustrated psychopathological experiences and symptoms. To conclude the analysis of the case, we can state that the W.'s psychoid puerility was the result of formally bringing to the present a melancholic biographic background, but whose content revealed an entire set of infant experiences which had been complexioned symbolically and crystallised in accordance with pre-established constitutional histrionic tendencies (21). With regard to that, we think that the anomalous personality traits can elect and favour some specific types of symbolic complexity, playing the role of a guiding and inducing axis for intense polarisation of certain experiences, whether real or imaginary (21).
After having concluded the theoretical discussion of the previous two clinical cases which we called psychoid states, it becomes necessary to recapitulate some of the attributes of those nosological entities we have established in another opportunity (18). On that occasion, we postulated a phenomenological standard of psychotic atypicality (18) which, in our view, can characterise those atypical pictures and can be summarised as the following: a frequent association between psychoid symptomatology and the presence of important traits or even a total personality disorder in the pre-morbid personality, besides the conception that the anomalous experiences of those pictures phenomenologically correspond to frustrated and abortive symptoms of classic endogenous psychoses (18).
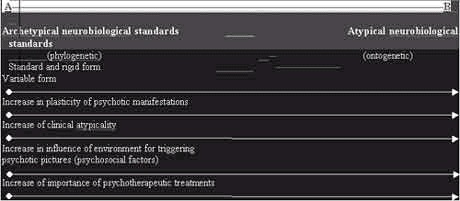
As a result, in order to achieve a dimensional and spectral view of endogenous psychotic disorders, we can consider the phenomenological standard of psychotic atypicality described above as a concept corresponding to maximum psychotic atypicality pole. We can visualise two axes and we name each according to the two respective concepts: pole A corresponds to the maximum degree of psychotic typicality and pole B is the maximum degree of psychotic atypicality. In other words, in pole A, we gather all those diagnosis criteria for the psychopathological characterisation of a schizophrenic psychosis, including its wisely unfavourable clinical development. In pole B, we place those atypical psychotic pictures, the psychoid states, which at times take hold of patients with certain personality disorders and display a rather benign and favourable clinical course. The two axes that configurate the two psychopathologically contrasting extremes of a psychotic spectrum have already been outlined as clear and diametrally opposite marks. So, how do we fulfil the space corresponding to the intermediate psychotic typicality spectrum? Which are the evolutive clinical-phenomenological general criteria clear and convincing enough for that?
At first sight, a rigid evolutive and clinical standard stands out in pole A, in contrast with pole B, in which a clinically multiform and atypical standard prevails, covered in a singular plasticity. Rigidity and plasticity, in our opinion, are terms which should correspond to well-defined neurobiological standards, mainly in the field of psychobiological studies of language phylogenesis (representation) Ù emotion. That correspondence will certainly interest the research on ethiopathogenic mechanisms and on psychopathological expression of what we now call psychotic pictures. Undoubtedly, the present researches focusing the biochemical mediations which complexly tangled in the various neuro-transmitter systems and the investigations confirming local brain disfunctions as causes of psychotic symptoms will forcedly converge on a definite postulation of basic standards, phylogenetically archaic (26), of relatively simple and rigid neurobiological structures up to those with enormous plasticity and flexibility, including in the psychopathological expression of atypical psychotic pictures. In fact, we can notice that, starting from a symptomatologically uniform and standard expression, as in the case of the classical forms of schizophrenic psychoses with its well-known psychopathological constellation and typical clinical development located in pole A, we move progressively into a gradually more rarefied sprectrum, concerning typicality, until we reach the point to visualise those psychotic pictures in which individual and ontogenetic psychopathological characteristics prevail, in pole B. We are then definitely detached from the rigid phylogenetic standard and now acquire peculiar characteristics, completely different from the former ones. Thus, in this journey towards the maximum pole of psychotic atypicality, we can see uncharacteristic, weird and incomplete experiences, as far as the classification of the psychopathological material is concerned, visualising atypical psychotic symptoms in a kind of detached way, as if abortive and frustrated, in those psychoid states in patients with personality disorder.
Therefore, we managed to elect some theoretical criteria for filling up the intermediate spectrum of psychotic typicality, namely, the psychopathological morphology, the clinical development and phylogenetic rigidity underlying the typical clinical forms in contrast with the ontogenetic plasticity of those atypical forms. This ontogenetic plasticity in turn implies an increasing importance of the unfavourable circumstances of the environment, that is, the psychosocial facts for triggering the more atypical psychoid states. In other words, the theoretical model suggests that the more atypical the phenomenological standard of a given psychotic picture, the more easily it is triggered by psychosocial facts.
The clinical similarity between delusional disorders and schizophrenic pictures (9,10,11,12,13) is remarkable, as there are delusional judgements in both (23,24). The difference is that, in the case of paranoia, there is a relative lack of phenomena such as hallucinations(26) and influential anomalous experiences, besides the integral preservation of the patient's personality entirety. In addition, delusional themes, generally about loss, jealousy and erotic-love, are strictly related to environmental and circumstantial aspects and perfectly fit the person's existential and cultural universe, that is, are consonant with his/her time, life, habits and view of the world. In contrast, in schizophrenia, it is common to find delusional themes totally disconnected from the intelligible heritage of common sense, as they have an archetypal and atemporal animistic-magic character (24). In paranoia, delusional judgements steeped in temporal and cultural-biographic intelligibility proliferate whereas, in schizophrenia, anomalous judgements also flourish, however, steeped in an atmosphere far more archaic and distant, full of cosmic and chthonic elements. The former refers to the animistic-magic individual-biographic and the latter to collective animism (24). The first is similar to a reified concretization of a well-connected and well-related individual myth while the second represents an abyssal and chaotic dive into the universality of the collective myth (24). One carries a predominantly ontogenetic reified content and the other conveys a exclusively phylogenetic reified representation.
As a result, it is reasonable to place delusional disorders immediately after the group of schizophrenias in the intermediate spectrum of psychotic typicality. They are followed by those psychotic pictures referred as schizoaffective due to the fact that, in general, they have an unfavourable clinical development resulting undoubtedly from the symbolic-affective dis-differentiation process (22), which takes place almost simultaneously with mood disorder. After that, it comes the delusional clinical forms of affective diseases, whether mania or depression, which despite their acute and productive aspect do not imply in damage or permanent and irreversible deficit of the symbolic-affective dimension, even in those cases which the phases succeed rapidly. It refers to those psychotic pictures which are generally well compensated by treating with lithium carbonate, valproic acid carbamazepine, isolatedly or associated one another.
After this we find the schizophreniform disorders with acute eclosion and favourable prognosis, which are many times well compensated by using lithium or any other mood-regulating agents. They are followed by the brief psychotic disorders and psychoid states in patients with personality disorders, also with fairly benign clinical development.
In order to aid comprehension, I believe the schematic diagram below can didactically summarise what has been discussed so far.
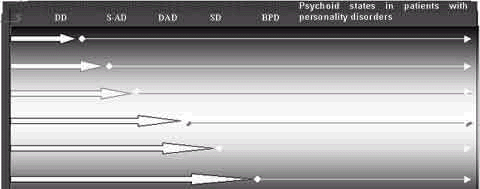

It can be seen that after Delusional Disorders (DD), it starts, from the schizoaffective pictures (S-A), a broad spectrum of psychotic clinical forms susceptible to treatment and control by lithium or other mood-regulating agents. Those pictures seem to consist in a real "spectrum of lithium psychoses", culminating in rather complex and atypical psychoid states, in which many times the therapeutic control is effective only if we associate lithium, valproic acid or neuroleptics at low dosages with antidepressants.
To sum up, it is plausible to say that the theoretical model discussed here ¾ represented by the diagram above ¾ in spite of being similar to a continuum, it is not intended beyond being useful to daily clinical practice, aiding the physician in diagnosing correctly and establishing a suitable treatment for his/her patients. It is my belief that the contributions which might help the diagnosis exercise in this clinical activity will never be excessive as the practice of Psychiatry is undoubtedly the most complex and difficult of all medicine specialisation.
REFERENCES:
1 - AKISKAL HS : The temperamental borders of affective disorders - Acta-Psychiatr-Scand-Suppl. 1994; 379:32-7
2 - AKISKAL HS : The prevalent clinical spectrum of bipolar disorders: beyond DSM-IV - J Clin Psycopharmacol 1996 Apr;16(2 Suppl 1):4s-14s
3 - AMERICAN PSYCHIATRIC ASSOCIATION - DSM-IV - Manual de Diagnóstico e Estatística de Transtornos Mentais, Porto Alegre, Publisher: Artes Médicas , 4th edition, 1995 (in Portuguese).
4 - AMERICAN PSYCHIATRIC ASSOCIATION - DSM-III-R - Manual de Diagnóstico e Estatística de Distúrbios Mentais , São Paulo , Publisher: Manole , 3rd edition, 1989 (in Portuguese).
5 - BUMKE, O. – TRATADO DE LAS ENFERMIDADES MENTALES, Francisco Seix-Editor, Barcelona, 1917 (in Spanish).
6 - FERNANDEZ, F. A. - "Fundamentos de la Psiquiatria Actual", Madrid, Editora Paz Montalvo, 1972 (in Spanish).
7 – GOAS, M.C – Temas Psiquiátricos, Editorial Paz Montalvo, Madrid, 1966 (in Portuguese).
8 - JASPERS, K. – PSICOPATOLOGIA GERAL, Livraria Atheneu S/A, Rio de Janeiro, 1973 (in Portuguese).
9 - KENDLER, K.S., GRUENBERG, A.M., STRAUSS, J.S. – An Independent Analysis of the Copenhagen Sample of the Danish Adoption Study of Schizophrenia – The Relationship Between Paranoid Psychosis (Delusional Disorder) and the Schizophrenia Spectrum Disorders. Arch Gen Psychiatry 1981;38;985-987.
10 - KENDLER, K.S. – The Nosologic Validity of Paranoia (Simple Delusional Disorder)- A Review . Arch Gen Psychiatry 37:699-706,1980.
11 - KENDLER, K.S. – Demography of Paranoid Psychosis (Delusional Disorder) – A Review and Comparison With Schizophrenia and Affective Illness. Arch Gen Psychiatry 1982;39:890-902.
12 - KENDLER, K.S., HAYS, P. –Paranoid Psychosis (Delusional Disorder) and Schizophrenia – A Family History Study. Arch Gen Psychiatry 1981;38:547-551
13 - KENDLER, K.S., WALSH, D. – Schizophreniform disorder, delusional disorder and psychotic disorder not otherwise specified: clinical features, outcome and familial psychopathology. Acta Psychiatr Scand 1995:91:370-378.
14 - NOBRE DE MELO, A.L. – PSIQUIATRIA, Atheneu Editora São Paulo S/A, São Paulo, 1970 (in Portuguese).
15 - MAYER-GROSS, W. – PSIQUIATRIA CLÍNICA, Editorial Paidos, Buenos Aires, 1958.
16 - PERUGI G; AKISKAL HS ; MICHELI C; MUSETTI L; PAIANO A; QUILICI C ; ROSSI L; CASSANO GB: Clinical subtypes of bipolar mixed states: validating a broader European definition in 143 cases - J-Affect-Disord. 1997 May; 43(3):169-80
17 - SCHNEIDER, K. – PATOPSICOLOGIA CLÍNICA, Editorial Paz Montalvo, Madrid, 1970 (in Portuguese).
18 - SOUZA, G.F.J. – A Fenomenologia dos Transtornos Psicóticos Atípicos – Os Estados Psicóides. Psiquiatria Biológica 6(2):99-106,1998 (in Portuguese).
19 - SOUZA, G. F.J. – "A Professora de História" - Jornal Mineiro de Psiquiatria, Year I, Number 1, Belo Horizonte, October 1997 (in Portuguese).
20 - SOUZA, G. F.J. – "Cenas Infantis" – Jornal Mineiro de Psiquiatria, Year II, Number 3, Belo Horizonte, February 1998 (in Portuguese).
21 - SOUZA, G. F.J. - "Considerações gerais sobre as Neuroses: Uma Visão Fenomenológico-Dinâmica", (unpublished), 1988 (in Portuguese).
22 - SOUZA,G.F.J. – The Endogenous Psychoses: A Phenomenological-Dynamic Approach, Belo Horizonte, 1990. Library at Heidelberg University - Germany, (in English).
23 -SOUZA, G.F.J. – A Fenomenologia Das Vivências Delirantes: Dois Casos Cínicos. Psiquiatria Biológica 6(4):98-201-210,1998 (in Portuguese).
24 - SOUZA, G.F.J. – Paranóia – Um Enfoque Fenomenológico e Antropológico, Temas- Teoria e Prática do Psiquiatra, 26(52):96-173-188, 1996 (in Portuguese)
25 - TALBOTT, J., HALES, R., YUDOFSKY, S. – TRATADO DE PSIQUIATRIA, Publisher: Artes Médicas, Porto Alegre, 1992 (in Portuguese).
26 - WILSON, E.O. – "Consilience – The Unity of Knowledge", Publisher: Alfred A. Knopp, 1998